Abstract
Resin Infiltration Technique on Enamel Opacities and White Spot Lesions (WSLs)
From Volume 47, Issue 6, June 2020 | Pages 536-537
Resin Infiltration Technique on Enamel Opacities and White Spot Lesions (WSLs)
Discoloration of enamel commonly occurs due to developmental defects, fluorosis and post-orthodontic treatment. Enamel discoloration can be an increasing aesthetic concern for patients. Conventional treatments include tailored oral hygiene, fluoride application and remineralizing agents in the first instance. Following this, more invasive options may be considered, including microabrasion and conventional direct and indirect restorations. The technique described shows the use of a resin infiltration system to improve aesthetics of white spot lesions to mask the appearance, prevent lesion progression and delay the restorative cycle.
Discolorations and white lesions in anterior teeth present as a management challenge, particularly in the younger patient. The use of destructive techniques creates a lifelong treatment burden and initiates the restorative cycle. Vital bleaching has been used with great success for the brown lesions seen in molar incisor hypomineralization (MIH) and fluorosis. The white lesions associated with these conditions and orthodontic decalcification, have historically required more invasive treatment. With the introduction of smooth surface resin infiltration systems, there is now a minimally invasive and pain-free approach that is a successful adjunct to the management of these lesions. Currently, only Icon (DMG, Hamburg, Germany) is on the market in the UK.
White spot lesions (WSLs) are localized areas of sub-surface demineralization under an intact enamel layer. This demineralization produces porosities which cause a change in the refractive index of the enamel.1 Risk factors can include poor oral hygiene, diet, salivary hypofunction, fixed orthodontic appliances and enamel defects.
White-spot lesions (WSLs) are the main iatrogenic effect of orthodontic therapy with fixed appliances.2 Nearly one-third of orthodontic patients develop at least one WSL as a result of poor oral hygiene and the retention of plaque around orthodontic appliances.3 The prevalence of MIH in European countries ranges from 3.6% to 25%.4 Further, a Cochrane Review in 2015 highlighted the prevalence of dental fluorosis of aesthetic concern was measured at 8% where there was 0.1 ppm of fluoride in the water supply, 12% at 0.7 ppm and 15% at 1 ppm.5
Most commonly, the first and most important conservative management approach is through tailored oral hygiene instructions, which in turn may remineralize the disturbed surface. Topical fluoride application may be beneficial, depending on the initial cause of the WSL,6 and also use of casein phosphopeptide amorphous calcium phosphate pastes. These approaches are, of course, dependent on patient compliance. More invasive treatment modalities may include enamel microabrasion or conventional direct and indirect restorations.7
Resin infiltration can be considered an alternative approach to prevent further lesion progression and improve the appearance of white spot lesions prior to considering invasive treatment. This can be both on localized enamel opacities, but also generalized opacities (Figure 1). The aim of this method of treatment is to occlude the porosities with low viscosity, light-cured resin which is achieved through capillary action. The resin has a similar refractive index to that of enamel and, as the resin fills the porosities, its appearance mimics natural enamel. This helps to improve the appearance of the WSL.8,9,10,11,12
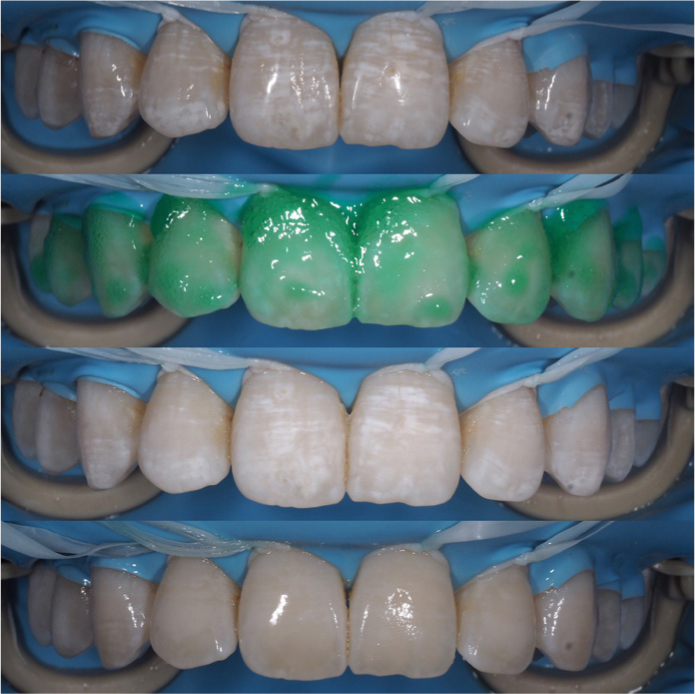
This technique tip describes the use of Icon (DMG, Hamburg, Germany) for the treatment of white spot lesions on the buccal surface of anterior teeth via resin infiltration.
The affected teeth and any adjacent should be cleaned prior to any treatment. This can simply be done with a prophy brush and paste (Figure 2).
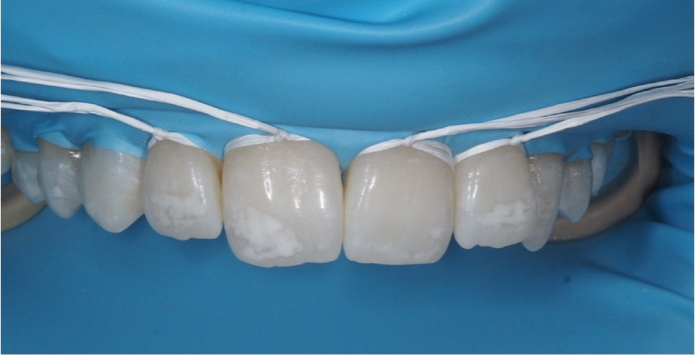
The teeth to be treated should be isolated with conventional rubber dam or liquid rubber dam. A bite prop or optra-gate may be helpful for some of these patients, particularly paediatric patients.
The lesions and surrounding enamel are treated with a generous application of 15% hydrochloric acid gel (Icon-Etch) and allowed to sit for 2 minutes. The gel can be gently agitated using a microbrush if necessary and washed away with water for 30 seconds. The aim of this stage is to remove superficial discoloration and the higher mineralized layer (Figures 3 and 4).
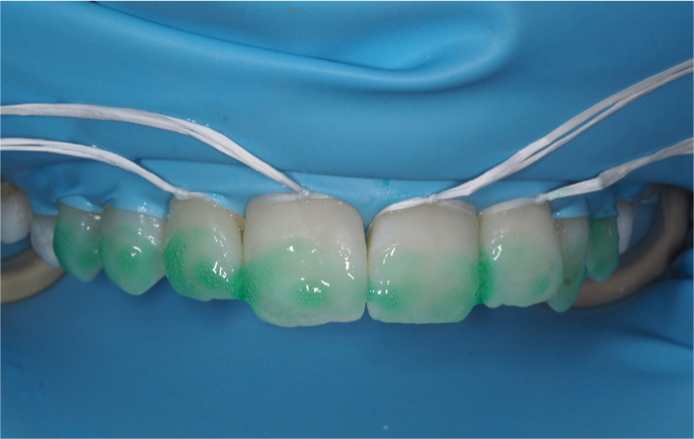
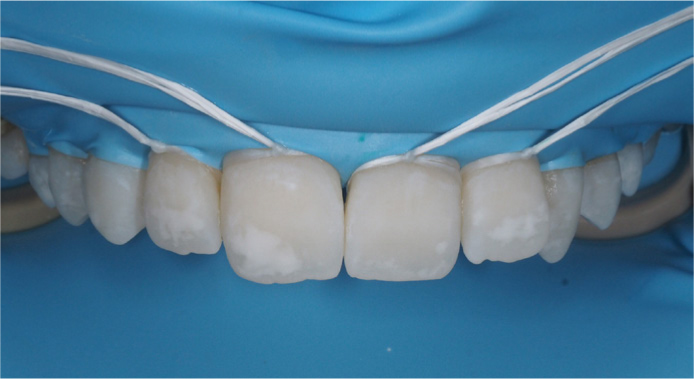
Next, a generous application of ethanol (Icon-Dry) is applied to the lesions and allowed to sit for 30 seconds. If the WSL is no longer visible, then it can be reasonable to assume that the lesion will resolve following the application of the resin.
Following steps 3 and 4, the white appearance of the lesions should fade. If the lesion is still visible, then steps 3 and 4 should be repeated until the lesion diminishes. If more than 4 repetitions are required, it may be that no further fading can be achieved and that another approach may have to be considered. It may be appropriate to continue with the suboptimal result and then revisit for what may be a less invasive composite than if a destructive approach had been taken from the start.
The methacrylate-based resin is infiltrated into the lesions (Icon-Infiltrate) for 3 minutes, excess can be removed and light cured for 40 seconds. This step can be repeated to reduce enamel porosity (Figure 5).
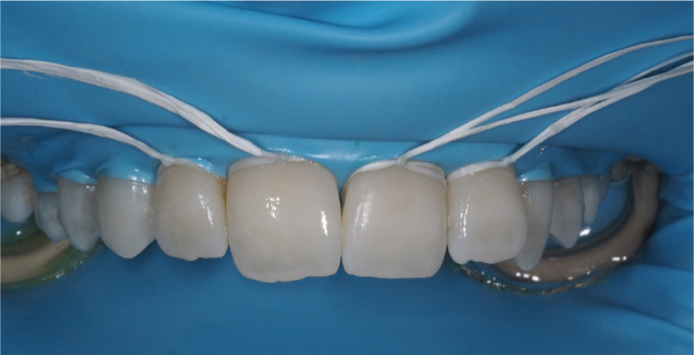
The rubber dam should be removed, and the surfaces of the teeth can be polished using polishing cups, wheels or discs, according to preference (Figure 6).
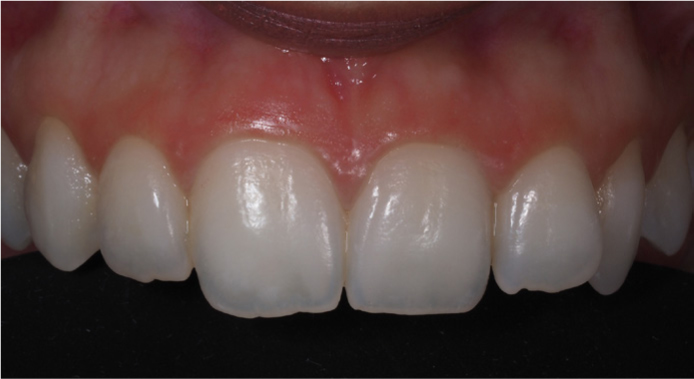
Resin infiltration is an alternative method for management of WSL, without taking an invasive approach. This treatment is particularly useful in young adults who have enamel opacities and defects. Given the increasing trend and focus on aesthetics, younger adults are more affected. Further, this gives the patients a minimally invasive treatment and allows for recovery of the natural tooth appearance.
Although straightforward, the majority of general practitioners do not offer this service. However, this is a treatment modality used in many specialist NHS paediatric and some restorative units; therefore, it is worth considering referral for these patients to a setting that is able to offer this treatment. In this regard, it is more important to try and avoid and delay the beginning of an invasive restorative cycle, particularly where there are other, more predictable options available.